TMS for OCD

Obsessive-compulsive disorder (OCD) is a condition characterized by recurrent, unpleasant intrusive thoughts and repetitive behaviors aimed at reducing anxiety or preventing some undesirable event. It currently afflicts between two to three million U.S. adults.
The condition is typically treated with some combination of cognitive-behavioral therapy (CBT) and a type of oral antidepressant called selective serotonin reuptake inhibitors. However, studies indicate that around half of OCD patients fail to respond adequately to the standard treatments. Moreover, many that respond to SSRIs discontinue due to undesirable side effects (e.g., weight gain, sexual dysfunction, emotional numbness, etc.).
Because of this, researchers began to search for novel treatments. Many focused on finding new applications for a non-invasive procedure called transcranial magnetic stimulation (TMS), initially approved by the FDA for treatment-resistant depression in 2008. In 2018, TMS became FDA-approved for OCD.
Here are answers to common questions about this new intervention.
What is TMS?
TMS is a drug-free and noninvasive procedure used to treat various brain disorders, including several mental health conditions. It uses magnetic coils placed just above the scalp to send magnetic pulses into specific regions of the brain associated with symptoms of the conditions it is being used to treat. For example, in the case of treatment-resistant depression, the pulses are sent toward regions of the brain associated with mood regulation.
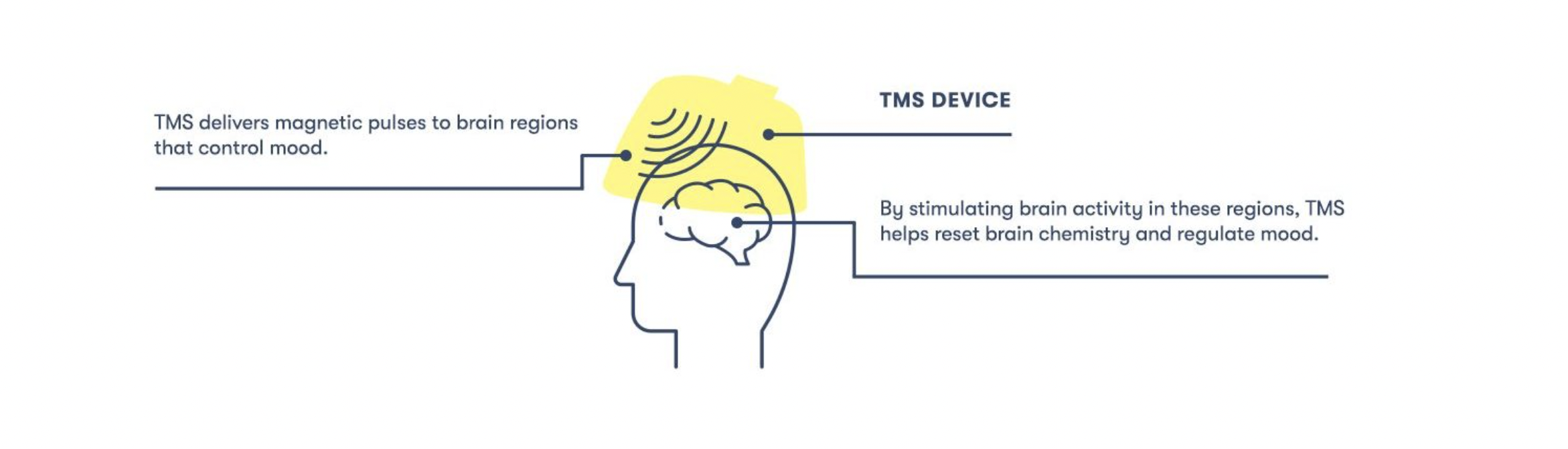
By sending repeated pulses to these specific areas of the brain, TMS “trains” neurons in those areas to fire differently and create new, healthier connections.
How Does TMS for OCD Work?
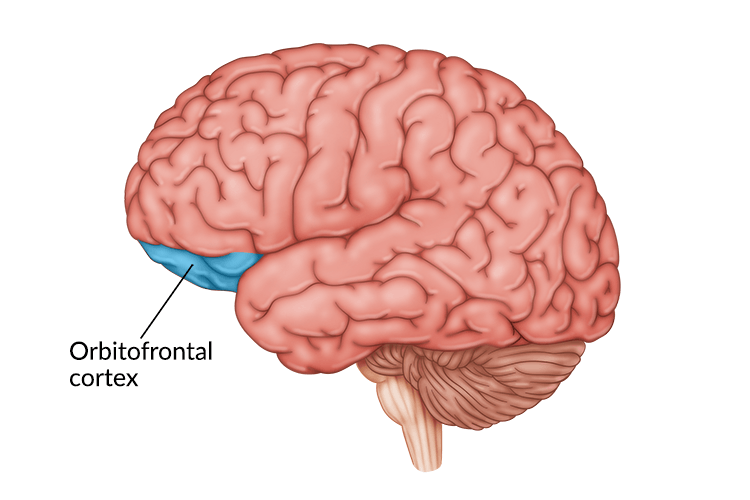
TMS for OCD works in much the same way as TMS for treat-resistant depression, except for two key differences. First, the magnetic pulses are directed at deeper structures in the brain, which are more closely associated with OCD. For example, one of the primary targets is the right orbitofrontal cortex, which studies have found is hyperactive in adults with OCD. It is also thought to be partially responsible for the unending urge to repeat compulsive behaviors that individuals with OCD experience. Other targeted areas include the supplementary motor cortex, medial prefrontal cortex, and anterior cingulate cortex.
Unlike treatment-resistant depression, which is associated with underactive neurons in parts of the brain related to mood regulation, OCD is connected with brain regions firing too much. As a result, in addition to targeting different areas of the brain, technicians utilize another type of stimulation called low wave stimulation, which inhibits, rather than activates, regional brain activity.
What are the Advantages of TMS for OCD
TMS has several advantages compared to the first-line oral medications used to treat OCD.
One of the problems with oral medications is that they are often imprecise, spreading throughout the brain and targeting many more areas than are directly implicated in the conditions they are meant to treat. This causes many unwanted side effects, such as weight gain, sexual dysfunction, emotional numbing, and more. TMS can deliver incredibly localized treatments, targeting the very source of the symptoms and avoiding unwanted side effects.
Aside from lacking precision, first-line oral medications often must be taken continuously to cause and maintain their therapeutic effects. After a round of TMS treatments, the benefits can last for a substantial period of time. On average, results last between four to fourteen weeks and can easily be sustained with quick maintenance sessions.
How Heading Does TMS for OCD Differently
In many cases, TMS is offered as a standalone treatment. While it can be very effective on its own, studies have found its effects can be amplified when combined with other interventions. For example, one experiment found that patients who underwent TMS and CBT experienced nearly a 60 percent drop in their OCD symptoms and that for 80 percent of the subjects, their symptoms decreased by at least 40 percent.
At Heading, patients have access to our integrated team of mental health specialists with wide-ranging expertise to complement their TMS and enhance its therapeutic effects. By combing TMS with other therapies, our patients benefit from the synergistic effects of a holistic approach to mental health.
Talk with your doctor to determine whether this treatment is right for you or schedule an appointment with one of our psychiatrists or therapists to advise you on this or any other potential treatments, including ketamine, Spravato, and TMS. Call us at 805-204-2502 or request an appointment here.
Want to find out if Heading is right for you?
Complete our consultation form and an intake specialist will get in touch.




 From recognizing one needs treatment to finding an in-network provider to scheduling an appointment, getting help for one’s mental health can be a time-consuming and disheartening process. One
From recognizing one needs treatment to finding an in-network provider to scheduling an appointment, getting help for one’s mental health can be a time-consuming and disheartening process. One 



 Mental illness is associated with various other chronic health conditions, such as heart disease and diabetes. Again, a longer DUI is associated with worse outcomes regarding many of these conditions. A 2022
Mental illness is associated with various other chronic health conditions, such as heart disease and diabetes. Again, a longer DUI is associated with worse outcomes regarding many of these conditions. A 2022