Can Ketamine Treat PTSD?

Post-traumatic stress disorder (PTSD) is a debilitating psychiatric condition caused by exposure to a terrifying or traumatic event. Individuals with PTSD may experience flashbacks, nightmares, severe anxiety, and uncontrollable or intrusive thoughts about the event. About eight percent of the population will experience PTSD over the course of their life. This condition is significantly more common among combat veterans, with nearly a quarter developing it during their lifetimes.
The standard treatment involves some form of psychotherapy, oral anti-depressants, or some combination. Many psychotherapies (e.g., exposure therapy, cognitive behavioral therapy, cognitive processing therapy, etc.) require patients to confront aspects of the traumatic event or how they think about it. While these therapies can be effective, they can also be stressful, causing many to stop treatment early.
The FDA has approved two medications, sertraline, and paroxetine, for the treatment of PTSD. These medications have several drawbacks. They take four to six weeks to start working. They also come with many side effects that lead many to stop taking them. Even when patients stick with the medications, only around 30 percent achieve remission. While other medicines have been used, the evidence for their efficacy remains questionable. As a result, there is a desperate need for faster, more effective, and more tolerable treatments for PTSD.
Why Test Ketamine for PTSD?
Over the past few years, ketamine has been explored as a potential solution. Researchers have turned to this medication for several reasons. One reason has to do with how ketamine acts in the brain. Ketamine is an N-methyl-D-aspartate receptor (NMDA) receptor antagonist. This means that it increases the amount of glutamate (a chemical messenger in the brain) and brain-derived neurotrophic factor (BDNF), which helps neurons grow and form new connections.
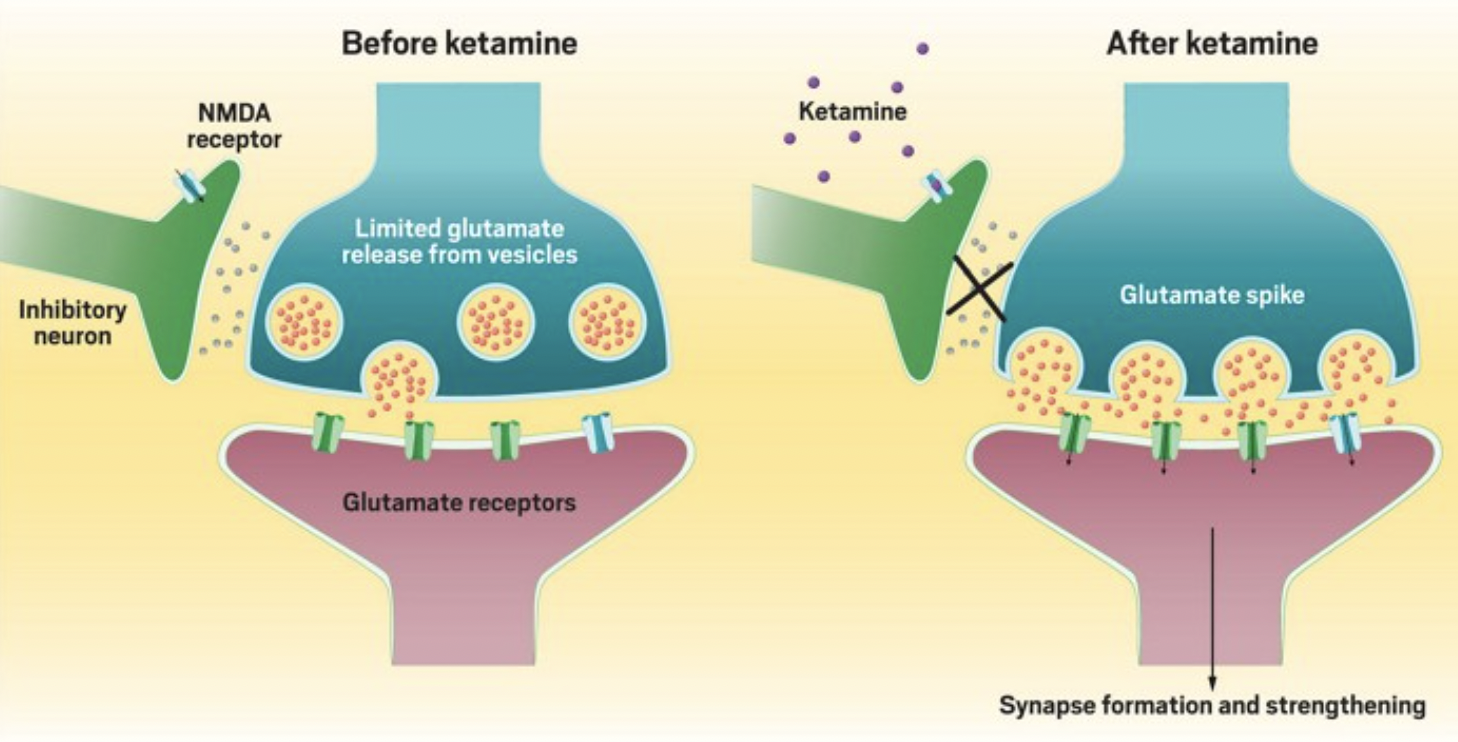
Early animal studies indicate that glutamate and BDNF play important roles in PTSD. One study found low levels of glutamate in mice exhibiting PTSD-like behavior after exposure to stress. Other experiments have found that several brain regions associated with fear and mood regulation had shrunk in mice after similar stress tests, suggesting BDNF might help rebuild these atrophied areas.
Ketamine is also well-established as a rapid-acting antidepressant. Since depression is a prominent symptom of PTSD, it should help with this part of the condition.
The Studies
Initial Experiments
With all this in mind, researchers turned theory into practice and began testing ketamine as a treatment for PTSD in human participants. In a 2013 study, an army veteran who was given a single infusion of ketamine experienced rapid and robust relief of his PTSD symptoms that lasted 15 days.
Following this finding, another group of researchers conducted a randomized controlled trial (RCT), meaning they gave one group ketamine and another a placebo. They found that PTSD levels were significantly lower in the ketamine group 24 hours after the infusion, and the effects persisted for around seven days.
Experimenters, hoping to extend the amount of time before symptoms returned, tried giving subjects repeated infusions of ketamine. In one study, patients received six infusions over two weeks. Eighty percent of patients achieved remission for 41 days on average.
Ketamine With Psychotherapy
 While 41 days is a significant amount of time, more sustained relief would be ideal. Instead of using more ketamine treatments, some researchers have explored whether the effect could be extended when combined with psychotherapy.
While 41 days is a significant amount of time, more sustained relief would be ideal. Instead of using more ketamine treatments, some researchers have explored whether the effect could be extended when combined with psychotherapy.
One of the commonly cited reasons for doing this is that PTSD is associated with deficits in what is known as “memory reconsolidation,” which occurs when a recalled memory is changed or altered in some way. Normal memories decay or degrade over time. Some theorists believe that for patients with PTSD, their trauma memories remain as clear and vivid as the day they were formed. Many therapies target this process of reconsolidation.
Ketamine is associated with neurogenesis. Recent studies have found that neurogenesis is important in reconsolidation. As a result, researchers have tested whether therapy might extend the effects of ketamine. One study which combined ketamine with prolonged exposure therapy found that after 90 days, the ketamine group had lower PTSD symptoms when compared to the group that received a placebo.
Prevention Vs. Treatment
Aside from comparing ketamine with and without therapy, researchers have tested its effects on PTSD when administered at different stages in the PTSD process. A recent meta-analysis compiled all the research on combat veterans and found some surprising results. Most notably, they found that when given during the early stages of PTSD (1-3 months after the traumatic event), ketamine exacerbated their symptoms. However, when administered beyond this stage, ketamine was consistently helpful. Exactly why the timeline is so important is unclear.
Conclusion
Ketamine appears to be a powerful treatment for PTSD. With that said, there are some caveats. When administered on its own, the effects are short-lasting. Repeated infusions can extend the benefits, but only to around 41 days. Psychotherapy may prolong the therapeutic results further, but more research will need to be done to confirm this. Lastly, the treatment may not work for all PTSD patients, especially those who experienced their trauma more recently.
If you feel you need to see a mental health professional or could use help deciding which service is right for you, please give us a call at 805-204-2502 or fill out an appointment request here. We have a wide variety of providers, including therapists, psychiatrists, nurse practitioners, and nutritional therapists who can see you in as little as one day via teletherapy.
Want to find out if Heading is right for you?
Complete our consultation form and an intake specialist will get in touch.

